Is Iodine Safe for Women with Underactive Thyroid or Hashimoto’s?
If you’ve been working to fix your thyroid, and reverse underactive thyroid symptoms or put Hashimoto’s into remission, you’ve probably seen the debates about iodine.
One practitioner says “iodine is absolutely essential for your thyroid.”
Another warns “iodine triggers Hashimoto’s flares.”
No wonder you’re confused.
The reality is that both too little and too much iodine can harm your thyroid, especially when certain nutritional deficiencies or insufficiencies are present, or if you already have Hashimoto’s or autoimmunity.
Let’s unpack this with the latest research, so you can support your thyroid properly and avoid common traps that can sabotage your progress.
Table of Contents
- Is Iodine Safe for Women with Underactive Thyroid or Hashimoto’s?
- The Vital Role of Iodine in Your Thyroid
- Why More Iodine Isn’t Necessarily Better
- The Gut-Thyroid-Iodine Connection
- How Much Iodine Is Too Much?
- How to Support Your Thyroid Safely
- When to Be Extra Cautious
- More Iodine Won’t “Heal” Autoimmunity
- FAQs About Iodine and Thyroid Health
- References
The Vital Role of Iodine in Your Thyroid
Your thyroid can’t make thyroid hormones without iodine.
Iodine combines with the amino acid tyrosine to create T4 (thyroxine), T3 (triiodothyronine), T2 (diiodotyrosine), and T1 (monoiodotyrosine), the hormones that fuel your metabolism, energy, mood, and more.
A healthy adult stores about 15–20 mg of iodine, with around 70–80% of that in the thyroid itself.
That’s why severe iodine deficiency causes goitre and hypothyroidism.
But this is rare today in countries like Australia, and the US, where iodine sufficiency is largely achieved through iodised salt, seafood, dairy, and eggs. In the UK, while iodised salt is available, iodine intake is usually obtained from foods such as dairy, fish, seafood, and eggs. Most people can meet needs through diet, but some groups, especially those avoiding fish and dairy, may be at risk of low intake.
Want to start supporting your thyroid with the right nutrients from the start?
My 7-Day Thyroid Meal Plan gives you simple, nourishing meals designed for women with underactive thyroid or Hashimoto’s.
Grab your plan HERE.
Why More Iodine Isn’t Necessarily Better
If you have Hashimoto’s, here’s what do you need to be aware of.
Excess iodine can:
- Disrupt gut microbiota: reducing beneficial butyrate-producing bacteria and increasing inflammatory TH17 cells (Virili et al., 2019).
- Trigger oxidative stress: inside thyroid cells leading to tissue damage and elevated TPO antibodies (Duntas & Doumas, 2009).
- Fuel autoimmunity flares: causing worsening fatigue, brain fog, weight gain, and thyroid swelling (Wu et al., 2006).
Women with Hashimoto’s are particularly vulnerable because their thyroid tissue is already inflamed, and sensitive to oxidative stress from excess iodine (Virili et al., 2019).
The Gut–Thyroid–Iodine Connection
Emerging research shows that iodine’s impact goes beyond the thyroid. It actively shapes your gut microbiome.
Excess iodine may:
- Alter microbial balance: reducing Firmicutes and Bacteroidetes species (Virili et al., 2019).
- Lower butyrate production: weakening immune regulation and allowing thyroid antibodies to rise (Cayres et al., 2021).
- Drive gut inflammation: which further fuels autoimmune activity in the thyroid (Cayres et al., 2021).
This creates a vicious cycle:
Too much iodine → gut dysbiosis → immune dysregulation → higher thyroid antibodies → more Hashi flares.
That’s why correcting gut imbalances and not just focusing on iodine supplementation is key to calming autoimmunity.
Many of my clients find that identifying gut imbalances, like infections, dysbiosis, or leaky gut can often be part of the cause(s) of their symptoms. If you’ve already tried eating right, various supplements, medications, and had lab tests done, but still feel lost and frustrated with your symptoms, you may want to look into supporting your gut with expert guidance. This is something else we can explore together inside my 1:1 programme, Energised Thyroid, or Behind the Numbers Reviews.
How Much Iodine Is Too Much?
The safe upper intake level (UL) of iodine for adults is about 1100 mcg/day (Institute of Medicine, 2001).
But for women with Hashimoto’s:
- Intakes above 500 mcg/day may trigger flares (Duntas & Doumas, 2009).
- Some thyroid support supplements provide 150–300 mcg per dose making excess intake easy.
Key risk factors for iodine excess:
- Daily seaweed use (kelp, kombu, wakame)
- Iodine-containing supplements or multivitamins
- Regular use of iodised salt and high-iodine diet
- Iodine drops or high-dose protocols (often promoted online, and can be unsafe for some with Hashimoto’s)
- Recent contrast imaging (iodinated contrast)
How Excess Iodine Can Affect Gut-Thyroid-Autoimmunity
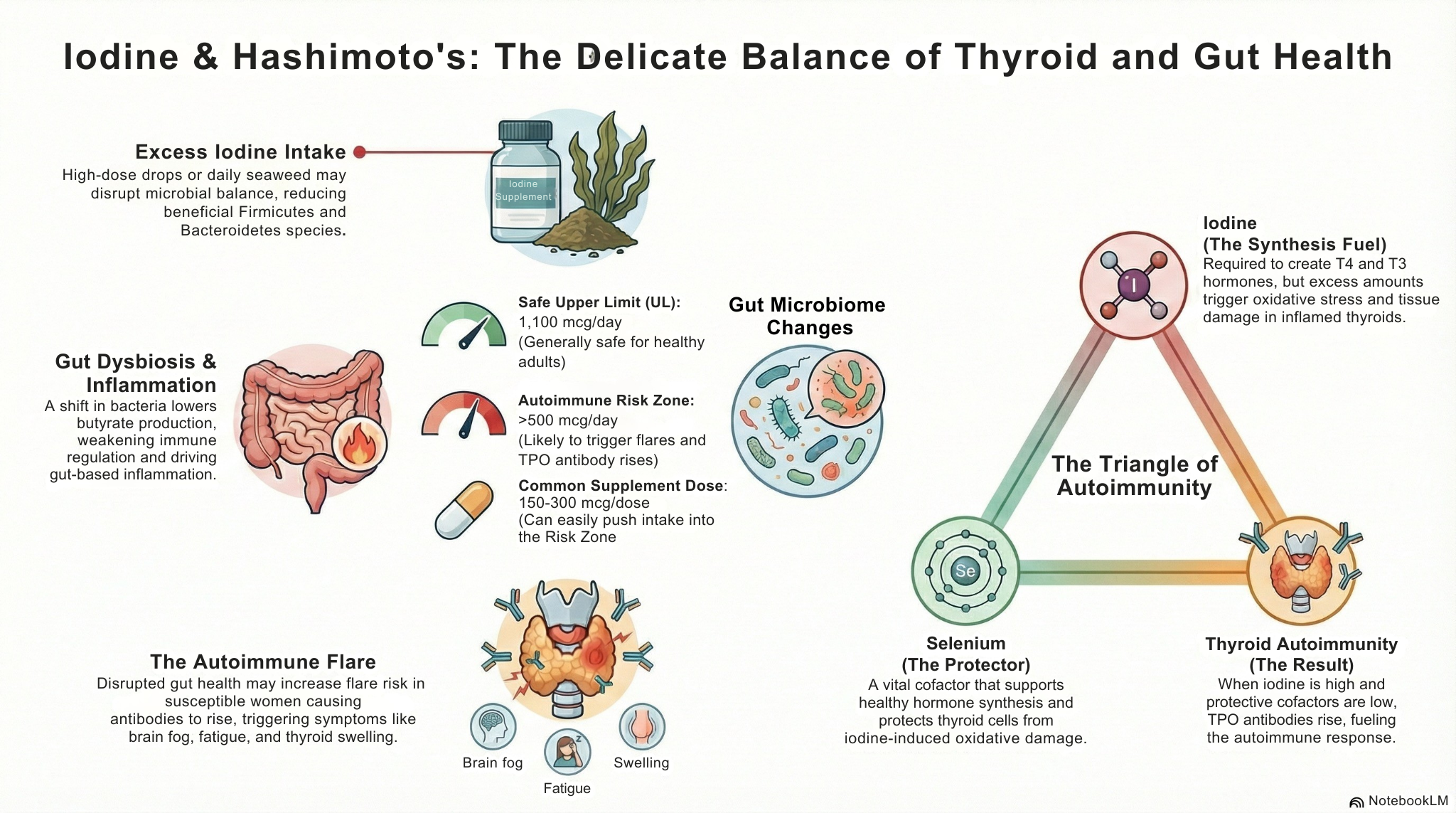
This is why I don’t recommend guessing with iodine, especially if you have Hashimoto’s, or high antibodies.
How to Support Your Thyroid Safely
Here’s how I coach my clients to navigate iodine:
- Test, don’t guess: start with a dietary and supplement review. Urine iodine testing may be helpful for some.
- Focus on food-first iodine: seafood, eggs, moderate dairy if tolerated
- Avoid seaweed supplements and iodine drops: unless clinically indicated
- Check all labels: including multivitamins and thyroid support supplements
- Prioritise gut health: support the gut microbiome and immune system balance
- Optimise cofactors: especially selenium and iron, which support healthy thyroid hormone synthesis and protect against iodine-induced oxidative stress (Duntas & Doumas, 2009).
When to Be Extra Cautious
- High TPO (>100 IU/ml) or TG antibodies
- History of thyroid nodules or thyroid cancer
- Pregnancy: iodine should be optimised before conception, with careful monitoring
- History of sensitivity or flares after starting new supplements
In these cases, it is wise to correct gut imbalances and support immune regulation first before considering any iodine supplementation.
More Iodine Won’t “Heal” Autoimmunity
Too many women with underactive thyroid or Hashimoto’s are misled into thinking iodine is the magic fix for their extreme tiredness and other symptoms.
But most thyroid issues are driven by immune dysfunction, gut dysbiosis, oxidative stress, toxins, infections, and nutrient imbalances, not iodine deficiency.
Flooding the system with unneeded iodine often backfires, triggering the very symptoms you’re trying to reverse.
The best thing to do is to calm your immune system, restore gut balance, eat foods that support you, and support your thyroid’s natural resilience, without overloading it with excess iodine.
If you’re experiencing constant fatigue, getting the basics (designed for women like you) in place first is the first place to start. Then you can layer in other types of support according to your needs. For many women, getting the foundations right is the first thing that helps restore the body’s natural energy production.
If you have Hashimoto’s and you’re unsure whether iodine is helping or making things worse, the safest next step is to review your symptoms, supplements, and thyroid markers in context. This is especially important if you have high antibodies, flare-ups, or you’re reacting to thyroid support products.
My Behind the Numbers review helps you make sense of your symptoms and blood test results, and decide on what to focus on next.
Learn more about Behind the Numbers HERE.
FAQs About Iodine and Thyroid Health
Is iodine harmful to everyone with Hashimoto’s?
No, but excess iodine is risky if you already have thyroid autoimmunity. Food-based iodine from seafood and eggs is generally safe; large supplemental doses are not.
How do I know if I’m getting too much iodine?
Check your diet: seaweed, iodised salt, dairy, eggs, and supplements all add up.
Testing urine iodine and/or doing a detailed dietary review with a practitioner can help clarify your iodine status.
Can iodine affect gut health?
Yes. Excess iodine disrupts gut microbiota, reducing beneficial species, reducing thyroid hormone conversion, and increasing inflammation (Virili et al., 2019; Cayres et al., 2021).
This is a key reason to avoid megadosing iodine in Hashimoto’s.
Should I take iodine if my antibodies are high?
Not initially, and only take if you’re found to be deficient. Correct selenium and iron first, address gut health, and work on lowering antibodies. Adding iodine too soon can worsen immune activation (Duntas & Doumas, 2009).
Is seaweed safe for thyroid support?
Occasional use is fine, but daily seaweed can easily push iodine intake too high, triggering flares in Hashimoto’s if you’re susceptible. Be especially cautious with kelp, kombu, and bladderwrack supplements.
References
Cayres, L.C. et al. (2021). Gut microbiota composition and gut–thyroid axis in Hashimoto’s thyroiditis. Thyroid Research, 14(1), 5.
Duntas, L.H. & Doumas, C. (2009). The ‘Triangle of Autoimmunity’: Iodine, Selenium and Thyroid Autoimmunity. Hormone and Metabolic Research, 41(9), pp. 581–586.
Institute of Medicine. (2001). Dietary Reference Intakes for Vitamin A, Vitamin K, Arsenic, Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc. Washington, DC: The National Academies Press.
Virili, C. et al. (2019). Gut Microbiota and Hashimoto’s Thyroiditis. Frontiers in Endocrinology, 10, Article 703.
Wu, T. et al. (2006). Iodine-induced hypothyroidism and autoimmune thyroiditis: animal and human studies. Journal of Clinical Endocrinology & Metabolism, 91(12), pp. 4501–4505.

